Episode #15 – Adrenal Fatigue, Part 1
Don't miss Part 2 and Part 3 (with Dr. Dan Kalish)!
Discussion Topics:
- Adrenal fatigue / altered adrenal function: what it is and basic physiology.
- What is stress? Types of stressors and their impact on our system.
- Signs & symptoms, bigger problems if it escalates.
- What to do about it: lifestyle factors, diet & basic supplementation recommendations.
View more graphics by listening via BlogTalk Radio.
Additional Resources:
- LISTEN TO Dr. Bryan Walsh's interview on Underground Wellness Radio and read his article on T-Nation.com “The Truth About Adrenal Fatigue” for some deeper science than I explained in the show.
- LISTEN TO: Chris Kresser's radio show here where he talks a lot about stress in the beginning portion of the show.
- READ: “Adrenal Fatigue: The 21st Century Stress Syndrome“
- READ: “Why Do I Still Have Thyroid Symptoms? When My Lab Tests Are Normal: A Revolutionary Breakthrough In Understanding Hashimoto's Disease and Hypothyroidism“
- READ: “Why Zebras Don't Get Ulcers“
Click here to download the episode as an MP3.
The episodes are currently available in iTunes, Stitcher & Blog Talk Radio.
[smart_track_player url=”http://traffic.libsyn.com/balancedbites/BB_Podcast_15.mp3″ title=”#15: Adrenal Fatigue, Part 1″ artist=”Diane Sanfilippo & Liz Wolfe ” color=”00aeef” social=”true” social_twitter=”true” social_facebook=”true” social_gplus=”true” ]LIZ WOLFE: Hey everyone, it's Liz and Diane of the Balanced Bites podcast. Welcome. Just a little reminder before we get started with our show today. The material and content contained in this podcast are for general health information only and are not intended to be a substitute for professional medical advice, diagnosis or treatment.
That's that. Diane, how are you doing?
DIANE SANFILIPPO:Hey, good. I'm excited. We have a good topic today. How are you?
LIZ WOLFE: I'm in the throes of an existential crisis, I think.
DIANE SANFILIPPO:Really? Uh oh.
LIZ WOLFE: Yeah, maybe more of a personal…like I never wear heels ever, and I wore heels today to the office and from the fricking car to the door, I've managed to injure myself somehow…
DIANE SANFILIPPO:Like this whole sentence that you've said, like or two sentences, like so many parts of that sound so wrong, like an office and heels combined. I don't even understand any of that.
LIZ WOLFE: I know. I'm fighting against myself here. I really, really am. I don't know. I just thought…you know, let's wear some tall boots today because it's kind of chilly out and people give me weird looks when I walk into the office, you know, barefoot and/or in Vibrams, so I figured let's knock some socks off. Let's wear some two inch heels. I have no idea where…I used to wear heels all the time, don't do it so much anymore. I don't know where I lost my ability to function in the real world, but it did happen and I'm crawling back into my hole now.
D:Yeah, Paleo cave welcomes you back. Take the shoes back and put on the Lululemon and let's, uh, yeah, be comfortable. I don't know. I know what you mean. Like I got dressed today and came out-like I got dressed today like a real person as I like to call it and went to the mall and did a couple things. I was okay, I'm wearing jeans and I was also wearing boots, but they were flat. And yeah, it felt weird. And I got home and completely changed into play clothes immediately, like sweatpants and…
LIZ WOLFE: Yeah.
DIANE SANFILIPPO:Like that stuff just…that stuff is just icky. I can't wear it all the time.
LIZ WOLFE: No good. I used to like it. I don't know what happened. I think my husband and I wear sweatpants. Like when I'm not wearing sweatpants, he's always like, Are you going to a funeral? or what-where are we off to right now? He's just….
DIANE SANFILIPPO:[laughs] He thinks it's fancy?
LIZ WOLFE: Mm-hmm.
DIANE SANFILIPPO:Oh my God.
LIZ WOLFE: Anyway, so that's where I'm at. That's my problem.
DIANE SANFILIPPO:Well, I'm back in sweatpants myself, so I can comfortably talk about our topic today, and I think that that will be welcome for everyone.
LIZ WOLFE: We'll go 90 and 10. You're 90 and I'm 10.
DIANE SANFILIPPO:Okay, all right. You'll ask the questions and maybe listener questions and your own questions, and we'll kind of get rolling. So I have a big glass of water here.
So what I want to talk about today is adrenal fatigue or we could call it altered adrenal function. This is the topic that I was really, really interested in, and I have been for a long time. I actually did a presentation-it was an hour and I have a bunch of resources for people who are interested in learning more and what I want to try and do is kind of demystify it a little bit. I think people get a little hyped up in whether or not they're diagnosed or something, but at the end of the day, most of these issues really all come down to diet and lifestyle as a primary sort of moving part and we can adjust a lot of things to help ourselves. So anyway, I want to get into some basics and then some ideas around what people can do, because I like to make sure people at least walk away from listening feeling like they have some action steps in their pocket. Sound good?
LIZ WOLFE: Sounds good to me. Yeah, so where do you want to start? Do you want to start by kind of explaining the beginning of all this?
DIANE SANFILIPPO:So..yeah, What I'm going to do I think is go through a few little science-y background things, you know. People can kind of listen to all of it and then pay more attention when I get to the sort of you know, signs and symptoms and what to do about it, but I do want to explain to those who are listening and want a little more science, a little more of the science and physiology behind it. Just so we're not speaking so abstractly, so I'll just try to go through a bit of these lessons and just, you know, if you want to stop and ask any questions that you have, I think a bunch of the questions that came in through Facebook all basically cover them, just while I'm talking. It's just kind of the natural progression of what this presentation and what this whole topic includes in term of how to identify it and signs and all of that. So yeah, I think I'm just going to kind of dig into it and start out with some of the background. Sound good?
LIZ WOLFE: Yeah, sounds good to me. I will sit back and drink some…
DIANE SANFILIPPO:Listen…
LIZ WOLFE: Lemon water and listen.
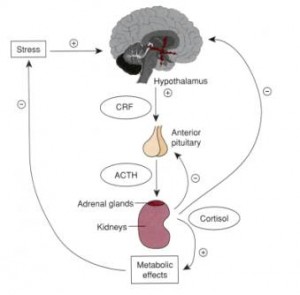
DIANE SANFILIPPO:Lemon water. Okay, cool. So the key players in the game between stress and adrenal fatigue before we get into sort of the what is it and all of that, just to lay down some key terms. Your adrenal glands are two endocrine glands that sit on top of your kidneys. Ad-renal, just meaning, literally they sit on top of the renal glands, so on top of your kidneys. They are responsible for producing and releasing cortisol. They also produce a couple of other things, but primarily when we talk about this situation today, we're talking about cortisol. Your hypothalamus-it regulates the secretion of a hormone called corticotropin-releasing factor, so that's regulated by the hypothalamus, and that hormone is secreted by the hypothalamus that signals the pituitary gland to release another hormone called ACTH, or Adrenal Corticotropic Hormone. So it sounds pretty complicated, but just to explain sort-they're all communicating with each other. It's not a matter of just your adrenal glands, just any one hormone. ACTH is secreted by your pituitary gland to stimulate the adrenals to secrete cortisol and other adrenal hormones.
Then we have the HPA axis, which is the Hypothalamus/Pituitary/Adrenal axis, so all of these glands are essentially communicating with each other in controls. It's a system of communication between the neuroendocrine glands that dictates our response to stress as well as our Circadian rhythm. So I'll mention the HPA axis a bunch when I talk about this topic, and essentially, what we're looking to do when we're looking to regulate stress response the whole idea of adrenal fatigue is really looking at the messages from our HPA axis, so all this is happening in our brain, even though we feel these responses n our body, in our energy level, etc.
And the hippocampus is the part of our brain that regulates the Circadian rhythm, and Circadian rhythm is an endogenously driven, roughly 24 hour cycle in bio-excuse me biochemical, physiological or behavioral processes. So essentially, it's your sleep and wake cycle. It's also regulated by part of your brain, part of this whole endocrine system. Again, it's called the hippocampus and that's what we're looking to make sure it's working properly when we're trying to make sure that we can be awake during the day and sleep during the evening. And typically that refers to daylight and nighttime, you know, daylight meaning sunlight and nighttime meaning darkness hours, so this is where we get a little bit sort of confusion when people are working night shifts. And I know that we've talked a little bit before, but it is pretty important as an overarching principle, that we're aligning ourselves with daylight and darkness.
So we just covered really briefly some of the key players. What is stress? So we talk a lot about stress on this podcast and we use the term very loosely and as a broad sweeping statement, but as it's defined, stress is a specific response by the body to a stimulus, such as fear or pain. It can disturb or interfere with normal physiological equilibrium. We talk about balance a lot, and everything we're going to talk about today with regards to stress is always about balance and how your body and brain perceive, translate, and react to a certain stressor. Stress can be physical, mental, or emotional strain or tension. It can be one situation or occurrence or stress can be a causative factor in other things. So some common stressors that people can associate with typically are things like financial stressors, death of a loved one, emotional stress, overexertion, lack of relax-lack of relaxation, sorry, something psychological. It can be a physical stress, like toxins, something like smoking or eating habits, sugar, refined food products, caffeine, coffee in general, but caffeine specifically in the coffee, artificial sweeteners. Negative attitudes or beliefs can be a stressor. Unwanted unemployment can be a stressor. Overexertion, the healing of wounds, prescription or nonprescription drugs. Marital stress, anything that's work related, any of that.
So these are kind of a list that I've gotten sourced from a book called Adrenal Fatigue. It's a really common book that you can check out by Wilson. Adrenal Fatigue. I think it's the 21st century stress syndrome, I think and so…
LIZ WOLFE: Yeah, that’s a good one.
DIANE SANFILIPPO:Yeah, if people want to check that one out. I have a whole bunch of books sitting here next to me, but really, that’s what we’re talking about when we say stressors. It’s not just one thing or another. So…hmm-mm. A little sip of some water. I’ve been yapping a bunch.
So the stress response, I think it’s really…I think it’s interesting and important to understand stress response, and I think that people can start to put their finger on what stress response feels like in some ways when you’re doing something like sitting in traffic, or you just-something scares you, and all of a sudden, you get that feeling of like your stomach dropping, you know? Or you get a skin response, like goose bumps? Something like that that kind of freaks you out, and you feel it. Physiologically, you feel that stress response, so we talk about like…we talk about inflammation and immune response in the gut really often. Feeling it is a digestive malfunction, right? We feel that gas, pain, bloating. That’s a very…Again, that’s like an extreme case of that stress response, that immune response in the gut. And feeling that, you know, stomach drop feeling, getting goose bumps from something that scares you, that’s sort of an extreme case of you feeling it. Stress response happens all the time in our body, just however we perceive something…some thought or action. And our brain and our entire endocrine system responds to the stressor. A stressor is any kind of input, what we just talked about, and then translated by your own perception. So two people can have a totally different perception of the same situation or the same toxin and the same input.
Your limbic system will respond to that perception of the stressor. It then sends a message to the hypothalamus. So we already mentioned what the hypothalamus does, and the hypothalamus, in response to all of this will send a message to your adrenal cortex-so the part of your adrenal system-or your adrenal glands, I’m sorry- the outer portion. Your adrenal glands have two portions-the inner medulla and the outer cortex. And the hypothalamus sends a message to the adrenal cortex that says, make cortisol. Okay, so, all of this is happening on a completely systemic level, and some of it happens in response to something that you literally-you know, you see it, you hear it, you think it, and if your body is responding.
So the adrenaline response is animalistic. You know, it’s the part of your brain that’s responsible for all of these emotional triggers and some of it is actually the response that you’ve actually conditioned over time. What happens in the brain is when we are used to responding to a certain trigger in a certain way, a phenomenon called plasticity causes the neurons in your brain to react in the same or similar way every time because it’s easier for your brain to react that way. So, you know, if you have a certain trigger, and it makes you sad or upset, and you kind of get that response all the time; similarly, you could be sitting in traffic every single day of the week, right? And then the weekend comes, and you’re actually not in a hurry, but you’re sitting in traffic again, and you have the same response. You have that response because your brain is so used to taking that easy pathway of telling your system this is a stressor we should get upset about, that you then get upset about it again, even though you don’t really have the same outcome on the other side. So it’s really important to understand that phenomenon because these are things that you can actually very, very easily control by changing your thoughts and changing the way that you respond consciously to stresses that exist.
Is this stuff making sense so far? I know, I’m kind of like yapping, but I want you to tell me if this is kind of making sense so far, Liz. And you can unmute yourself.
LIZ WOLFE: I won’t interrupt, if I want you to add something in there because I have a feeling that you’re going to get to most of what I would say. So I like it so far.
DIANE SANFILIPPO:Okay. All right, we can move back around any of this, but I definitely, you know…If you do have something that you want to ask me, go for it, because I’m just going to keep going.
Okay, so that’s just kind of a basic of a stress response and understanding that you can feel it in some ways, and it’s also happening underlying the same way systemic inflammation might be happening. And sometimes you feel it and sometimes you don’t, and it comes out in different ways. So we’re kind of building up to talk about this. Hmmm?
LIZ WOLFE: I have a comment real quick.
DIANE SANFILIPPO:Yes.
LIZ WOLFE:Just to kind of tie this up with the other idea of other hormonal functions, and you can kind of tell me what you think about this, but, when we look at like insulin kind of as an averaging hormone…Basically, the nature of hormones in general, and like you’re saying how you kind of have a conditioned response to certain things that manipulate your hormonal environment. I think maybe, you know, we can kind of draw lines between this and blood sugar disregulation, and even metabolic syndrome, just looking at how you don’t have an exact reaction to the exact stimulus every single time. If that makes sense. Like, you put together, over time, kind of how something is going to be reacted to. So while you may have a slightly different stressor, you may react to it in the same way. Does that make sense? Hormones kind as a conditioned mechanism?
DIANE SANFILIPPO:Yes, absolutely. As a conditioned response at a certain point…it almost gets to a point where this is why sometimes when people do start to change their habits, it’s difficult and painful at first because their body is really conditioned to responding to old stressors, and so it can be painful to make changes in those inputs. Does that make sense? We’ll talk a little bit more too about blood sugar and how like the rest of hormones come in because that’s kind of our…when we talk about symptoms of this?
LIZ WOLFE: Mm-hmm.
DIANE SANFILIPPO:That’s where that kind of starts to tie in to make sense.
LIZ WOLFE: Cool.
DIANE SANFILIPPO:So like super…again, to recap, there’s physical or mental and emotional stress. Physical stress can be what you were talking about-some other, you know, hormonal imbalances. Blood sugar imbalances. Food allergies and intolerances. Poor food. Lack of sleep. Caffeine. Inflammation, which we talked about a bunch a couple weeks ago. Chronic illness. Training and exercise. And a lot of those physical stressors can be at a systemic level you are not perceiving daily, so that’s one of the things when I talk about detecting adrenal fatigue or an altered adrenal profile, sometimes you don’t know what’s happening because it’s at a systemic leveLiz Wolfe: some kind of infection, some kind of issue with your body that’s causing the symptoms. But it’s not like, you know, you might be putting yourself to sleep every night, eating a perfectly clean Paleo diet, and you still have something going on. Mental and emotional, you guys can remember all the stuff I talked about already. Anything that’s kind of beating you down, mentally and emotionally.
So what are some symptoms of an altered adrenal profile? And that's-you know, it really hits home for me as I've been dealing with this recently. I've probably dealt with it for years, but in different ways it's affected and in the last year or so, it's been affecting me so greatly, just with starting a business and doing all this stuff from the ground up that I finally am really doing a lot more about it. So I'll talk more about you know, protocols or at least some supplementation that people can look at, but some symptoms would be, probably the most obvious, fatigue, headaches with physical or mental stress, weakened immune system and allergies, getting, you know a really slow start in the morning, gastric ulcers, headaches in the afternoon, that really, really exhausted feeling in the afternoon, feeling full or bloated. And that's not just satiety from a meal, but just sort of this unidentifiable, you know, bloat. Craving sweets, caffeine, cigarettes; blurred vision would probably be a more advanced symptom. Unstable behavior. becoming shaky or lightheaded if meals are missed or delayed, which again that ties very, very closely to blood sugar disregulation. If you can't stay asleep or fall asleep. Dizziness when you're moving from sitting to standing or lying down to standing. Transient spells of dizziness. Any of that. Asthma. And then hemorrhoids, varicose veins. Those could all be signs of an altered adrenal profile.
A lot of these are taken from Dr. Datis Kharrazian's book Why Do I Still Have Thyroid Symptoms When My Lab Tests are Normal? A really excellent book for anyone's who concerned about their thyroid, and the reason that that's in this book is that your entire endocrine system works in a cascade. So blood sugar regulation is always primary to dealing with adrenal issues or dealing with thyroid function. If your insulin regulation is poor and blood sugar regulation is poor, then your entire endocrine function will be sort of set up on shaky ground. Every additional course where I've gone to and I'm sitting in a lecture learning about any, you know, brain chemistry, endocrinology, gut function, any of that, blood sugar regulation is always first and foremost what the person needs to address because if your blood sugar is up and down on a roller coaster all day long, then your insulin levels will be chasing that all day long. We can't look at fixing your adrenal function if your endocrine function is so stressed by the insulin response you're asking it to make by the food that you're eating. So that's kind of why all that stuff really matters, that's why you and I really take the approach of sort of the ancestral diet, getting away from the refined food, because we're going to start to put the kibosh on a lot of the initial triggers for this stress response by evening out our blood sugar and insulin levels.
Additionally when we talk about reasons why this whole adrenal stress thing are so important, it's because of the secondary cascade of hormones after adrenal function. So it's almost like, yes, I care that people are not stressed out or tired and wired, but I care more that it doesn't progress into something like infertility, that it doesn't progress into PCOS, low libido, depression, anxiety, and as I mentioned before, thyroid disorders. When we look at the cascade of hormones, and I'll throw off just a really basic chart in the podcast notes that people can look at. When you see what happens, and anyone who's been to my seminar has gotten a taste of this to learn how this works, and all this actually-all this hormone production does actually start with cholesterol, right? Which is why we love people having healthy, robust cholesterol levels in a healthy range because in order to make hormones, we need the substrate from cholesterol. When a person is experiencing a chronic stress response, the body can start to funnel hormone production to stress hormone and ignore a lot of the sex hormone production. People may have heard of this before; It's a phenomenon called the pregnenolone steal , where essentially your body's critical function is to survive, it's not to thrive and reproduce. It's literally just fight or flight, let's survive, fight this tiger, run away, stay alive. It's not going to be concerned with whether or not your sex hormones are very balanced, so this is where the things like infertility, PCOS, depression, anxiety, and thyroid disorder start to come in, is that your body is really focusing on “we're in a stress response, we're focusing on staying alive and producing these hormones.”
Are we kind of making sense so far?
LIZ WOLFE: Yeah, I like it. I think just to kind of pull out something that we're kind of mentioning a little bit. I think that a lot of people may confuse long term blood sugar disregulation type of indicators with adrenal fatigue, which is fine because I think in both situations the approach is often the same. But I just want to say, don't necessarily be so fearful that your adrenals are shot when you can potentially take a step back and look at your ability to handle sugar and kind of a long term approach to that as well, but I think you kind of covered that.
DIANE SANFILIPPO:Yeah, no, but it is a good point, and that's why when I talk about steps to kind of work on this. Working on blood sugar regulation is always going to be first and I actually think you need to do it for awhile before you address figuring out whether or not if your adrenals are the problem. So when I talk about what's next in terms of the perception vs. the reality I think that will start to become more clear, and then have me loop back around the blood sugar stuff if it's not clear yet again later. Cool. Okay.
So I started this to approach this topic in a different way from how I originally learned about it years ago to what I've been reading more recently in the last couple of years. What I originally had learned was a standard approach that people go through stages of adrenal fatigue or adrenal exhaustion in that you need to be first, having a response of demanding a high level of cortisol production. And then after that, you start to tap out to where you have lower production, and overall it's just low, you know. It's not flatlined, but it's just kind of looking like your adrenal tests that come back will be kind of low overall. And then there's another stage where your morning levels might be kind of low, and your evening levels will get high, and that will be opposite of what you want. You want your morning levels of cortisol to be high. You want to be awake and alert in the morning. And in the evening, they taper off so you can go to sleep. Melatonin starts to kick in as a counter-regulatory hormone to cortisol. If you're experiencing something where in the morning, it's very low and in the evening it starts to get higher, that's what we call a “tired and wired” state. And then the fourth stage would have been, and I think this is stuff that Wilson talks about in his adrenal fatigue book, is that it's pretty low, flatlined overall, potentially sort of the rock star phenomenon, where you literally are so exhausted that you pass out. So that's kind of you know, that's kind of the standard approach that people were taking, that you might need to pass through stage 1 before you get to stage 2.
Some of the studying that I've done in the last couple of years, a really good article that people can read by Dr. Brian Walsh is on T-Nation.com, and also he's got a bunch of information just on his website, drbrianpwalsh.com. He's got interviews with Sean Croxton at Underground Wellness that I think people should check out. But I think that his take on this whole subject is really the best I've seen so far and the one that makes the most sense to me. In especially what we see clinically and in our, you know, practices and with our clients, you know we're not necessarily seeing people who have gone through all these different stages. You may actually present symptoms or test results-adrenal stress index test, which is a saliva test-results that put you in one stage or another, and it doesn't mean that you had to go through each of those stages necessarily.
So what I want to clarify now is some of the perceptions that people have and then what the realities are.
So one of the perceptions is I think is that when you're experiencing this notion of adrenal fatigue or an altered adrenal profile is that your adrenal glands aren't producing enough cortisol. But the reality is that it's very rare for your glands to stop producing hormone. That might occur in something called hypoadrenia or Addison's disease, which is an autoimmune condition. That's a similar thing to like an autoimmune condition like a thyroid condition, where the thyroid is actually not making thyroid hormone anymore. It's very, very rare. What's actually happening is that you know, the perception that people have on the other side is that your adrenals might be putting out too much cortisol in response to the stress. Well, the whole idea here is that your adrenal glands literally do what you tell them to do. They're getting their marching orders from the hypothalamus, from the HPA axis. They're getting their marching orders-they make the cortisol. They don't actually have a brain. They don't know what to do with this cortisol until the message is sent to them from your hypothalamus saying, Hey, here's how much cortisol we need to respond to whatever stressors are happening. So the perception has been that by simply addressing the adrenal glands, we could overcome the adrenal fatigue. People think that things like, you know, vitamin C and B vitamins and even taking things like adrenal glandular supplements, just supporting the problem, might fix the problem. But it doesn't fix the problem because the problem isn't the adrenal glands, it's not that they can or cannot produce cortisol; it's the messages that they're being to sent to put out at any given time.
So now that I've said that, how do we address what the messages are that our brain is sending to our adrenals? Well, this whole thing is really based on a balance of neurotransmitters. And so this is where it starts to get a little, a little science-y, and I'm not going to get into a list of a million neurotransmitters, but I'm going to explain just kind of briefly how this balance works. And you can kind of picture-the way that Brian Walsh explains it, he pictures-he asks you to picture like a funnel of messages coming in. I think a teeter-totter is a good visual, because we're always trying to strike a certain balance and you know, we say this with a lot of different body systems. But I think when it comes to the messages that our brain is sending to the rest of our body, I think it's important to just picture this teeter-totter and your hypothalamus is sort of that flatline of the teeter-totter, and on either side, you've got different neurotransmitters.
Some are called excitatory neurotransmitters, some are called inhibitory neurotransmitters. So different neurotransmitters that we might have can be things like GABA, which is an inhibitory neurotransmitter, or something like MSG, which is excitatory. Things that will affect these messages include our hormones themselves; cytokines, which are systems from the immune-er, signals from the immune system; lipopolysaccharide, which some of you may have heard Robb Wolf's podcast-I think he's talked about it or Mat LaLonde talked about them, they're waste or endotoxins from bacterial infections. Gram negative bacteria. All of this stuff can affect this balance. So when we talk about things that are more excitatory, they will inhibit the immune system. They will cause high blood sugar or insulin resistance, and they tell our system, make more cortisol. So anything that's giving me a more excitatory response says, make more cortisol you know, lower immunity, push the blood sugar higher.
When we've got the flip side of that, we've got the inhibitory message that say, enhance the immune system, lower blood sugar, you know. Make recovery from work outs a little bit longer. That sounds like you know, it sounds like people might try and decide which is better or which is worse. Do we want more excitatory? Do we want more inhibitory? And, you know, kind of the whole point of this is, it's not about having more of one or the other, it's about the balance between them because as neither is good or bad, we need both. The same way we need both omega-3/omega-6 fatty acids, to have pro-inflammatory and anti-inflammatory responses. It's about getting these messages balanced, and so typically, we need to find out what messages people are receiving too much of. A lot of times people are getting too much of the excitatory neurotransmitters. They're having this sort of anxiety response, they're, you know, they're nervous all the time, they're feeling that heightened sensation of that nervous stomach, and they might need things that are more inhibitory to calm them down. Some people are not experiencing that. Some people are actually, you know, experiencing low blood sugar. You know, they're hypoglycemic, and they might need something to push that a little bit higher. People have asked about-I saw on the Facebook page, people have asked about like low carb diets, and, you know, could carbohydrates be helpful or harmful in this adrenal situation? Well, that's where some people who are experiencing this phenomenon actually having too low of a carbohydrate intake might be worse for them. They might need to raise their blood sugar a little bit because they're experiencing too much of that low blood sugar.
So it really all depends. Every single person's system and reasons for having these problems will be different. There is not one “here's why you might be experiencing this” that will be fitting every person because every single person….I could have a room full of 30 people de3aling with some sort of state of altered adrenal profile, and you know, maybe a third of them hate their job. Okay that's going to push their brain chemistry in one direction. Maybe a third of them have, you know, kids and family that are very stressful for them. Maybe a third of them have an autoimmune condition that's pushing their own body chemistry around in a way that they can't actually make an exact control over. So we all have different things that will push this around for us, and we all need to take stock of what might be balancing our brain chemistry, one way or another.
So when we talk about figuring this out a little more, we can at least, you know…Liz, one of the things you had asked about is like okay, well, could it just be that the person is experiencing blood sugar disregulation? Absolutely. There could be a lot of things happening that are not really rooted in this adrenal issue that can all affect your adrenals. So a couple of things that people can do to test or assess whether or not they have this adrenal stress. The very best way to do it would be to get a salivary adrenal stress index. This is a saliva test that is measured 4 times over the course of the day. Some people say it might not be that accurate because you know, day to day, it might be a little bit different. I think for the most part, it's probably the best thing that we have-the best tool that we have to test it, depending on what kind of investment you can make. They're typically $130 to $150 for each one that you do. I would recommend that if you're concerned about this, you know, you deal with a lot of the diet and lifestyle factors first, and then you look into an adrenal test. So that measures your saliva's cortisol levels over the course of the day. Pretty accurate. I run those tests through a lab called Metametrix. There's a couple of other at-home tests that people can do. There's a pupil reflex test that people can do by shining-turning the light off in the bathroom, looking in the mirror, and shining a flashlight into the pupil of one eye. And it should contract as you would expect. If after around 30 seconds, it stays the same or it begins to dilate, you might have some adrenal fatigue. So basically it's your body's response to that flashlight can't hold strong, and your pupil starts to dilate again and get bigger, then you might be dealing with some adrenal fatigue. Then there's also a postural test, and you can kind of just Google these and find some more details around how to do it. But essentially, it's a blood pressure test where you take your blood pressure while you're sitting down, and then stand up and immediately test your blood pressure again. If the systolic number, the first number, didn't raise by 8 to 10 points, then you might have an issue. If it dropped, you probably have some fatigue going on. So the first number should raise by around 8 to 10 points. If it didn't, that's noteworthy. What else can I tell you about this?
So really the baseline for looking at trying to heal your body, and I'm going to talk a lot more about some of these recommendations. When you remove refined foods, when you're focusing on sleep, when you're trying to do some smart exercise and not overdo it, those are the first steps. Getting all of the stressors that you can-that you know about-like if you know you're eating garbage food, that's stressing your body. Stop doing it. If you know if you should be sleeping better, get your sleep hygiene in check, sleep in a dark room, turn the computer off early enough so that it's not stimulating your brain too. You know, do all the things you need to do to get yourself in bed. What you might find is that you lay there, and your mind is racing. If you've done everything you know to do, and you've done that for several weeks, where you're getting that hygiene intact, where you're turning lights off , you're maybe taking a warm bath or shower, you know, you're not going to bed too hungry-maybe have a little bit of protein with a little bit of carbohydrate, help the tryptophan from your protein cross the blood-brain barrier and calm you down.
Like all these different things I've talked about before, but if you find, and this is what happened to me, I was laying down and my sleep wasn't good. Like, I would fall asleep and I would wake up two hours again, and again two hours later, and would constantly be waking up during the night. And you know, as a practitioner, and I think a lot of us do this, I tried to do everything I knew I could do before I turned to testing and supplementation. Because just like with any other problem that kind of might come up-say something arises and I need antibiotics or some kind of prescription medication, I want to know that I'm addressing every possible outlet that has to do with diet and lifestyle first, and if somehow those factors won't fall in line. If I'm doing what I know to do to regulate my blood sugar, and it's still not regulating, then there might be something else going on that I can't exact control over and I might need some help from supplementation. So that's kind of where I got to at a certain point. I took a test. My adrenal profile came back overall pretty low output. And slightly tired and wired, which if you kind of read over the stuff that Brian Walsh talks about, this kind of really hit home for me when I heard him say it with that…if he had an altered profile where he was low in the morning and high at night, that would be the biggest thing he would be focusing on because that's one of the things that sort of the known carcinogen. That disregulated hippocampus signaling that's addressing our circadian rhythm, that's when we have the real problem of a carcinogen. And so you know, we're looking to keep ourselves healthy and avoid things like cancer if we can. So if I'm tired and wired, you sure as heck better believe that's the first thing I want to address.
With the different types of adrenal dysfunction as I've mentioned, you know we can categorize them in stages. We just may or may not be passing through different stages at different times. You could have a chronic infection that puts you into one stage or another. You could have an acute infection. Something like pneumonia could instantly put you at low cortisol output just because it's lowering your immune response. So these different things can happen at different points. But stage one again is that alarm stage: anxious, nervous energy, chronically high levels of output. Stage two is low; it's called the resistance stage. The output is low, but you still have some function. You've got stage three where you're kind of always tired. Low energy, but you might also have that disregulated rhythm, and then the exhaustion stage. Disregulated rhythm can also kind of come at any time. But I think for the most part, people might tend to see that as sort of like a stage three, when you're tired. You're going to probably get some kind of peak at some point.
Some of the signs that people might have or some altered adrenal function outside of just some of the physiological symptoms, but some of the lifestyle signs literally hitting the snooze butter a million times in the morning.
LIZ WOLFE: wow.
DIANE SANFILIPPO:You could be dealing with this problem. [laughs] Now we're talking? You know, you can't get yourself out of bed. Somebody who-and I think we all have seen this-somebody who literally is drinking coffee all day long, or some kind of caffeinated beverage all day long because they can't stay awake. That might be a sign that you're dealing with this. When it comes to exercise, yeah, you should be tired after you work out. But like, about 20, 30 minutes later, you should be feeling fine, like you know, maybe your exercise-your workout was hard for that 20 minutes or so, you know, like a lot of people are doing like high intensity stuff or CrossFit type workouts or lifting. So yeah, it should take something out of you for that moment, but you shouldn't be beat down for the rest of the day from that workout. You should be able to bounce back from that within that 20 to 30 minutes. If you feel beat down for the rest of the day, that workout was too much for you and you're probably dealing with some fatigue issues. That's where you need to look at what's happening with that workout and decide what is it you can attack or not.
You know, I've been trying to recover myself for the last like two months now on a protocol, and I had a weekend where I taught…I came home. I moved back here like on a Wednesday, taught a seminar, so that was a cross country flight on a Wednesday, taught a seminar on Saturday, so that's me all day, outputting energy, you know, at my 110% energy, and went to my high school reunion that evening. And then the next morning, I did a workout, and I planned on just lifting weights that morning, and what I ended up doing was like a 30 to 35 minute, you know, moderate level MetCon. And I'll tell you, I was dead the rest of the day. I was tired. I took maybe two naps that day. That was too much for me. And I knew it was going to be too much, but I tried to just take it at a moderate pace and not, you know, kind of go balls to the wall, you know, as some might say. Like I really wasn't trying to do it super fast, but it was really too much for me. And I think, you know, not everyone's in that place. But if you are, it's a really big sign that you need to be training and not draining yourself, and that's something that Paul Chek says a lot. Are you training or draining? And it's not about going and literally gunning yourself and leaving it all on the gym floor. It's about doing things that are going to be anabolic and building capacity in your body, and if you're literally doing things that are catabolic or breaking you down that whole time, especially if you're fatigued, it's not producing any sort of positive effect.
So what other questions, you know, do you think kind of pop up from that so far before I talk about addressing this, some lifestyle factors to work on that I've already mentioned some of, and then some other issues about what to do? What other questions do we have from Facebook or anything that you've got on sort of the issues surrounding where this comes from?
LIZ WOLFE: Looking at these Facebook questions, which were awesome, I think you actually covered a ton of the answers already. But talking a little bit about exercise…We had a question that sad, like you just said, “Is it true that some forms of exercise can actually make it worse?”
DIANE SANFILIPPO:Mm-hmm.
LIZ WOLFE: And it does sound like obviously, if you're dealing with a certain amount of fatigue, you do need to be careful about the volume and intensity of your training. But I guess along the entire spectrum of exercise, are there workouts that can actually induce adrenal fatigue, or is that a total lifestyle thing, like we've been talking about? You've got to have the emotional, the physical, the environmental stuff?
DIANE SANFILIPPO:So I think that's a good question. I absolutely think there are exercise forms that can induce this. I think that my sort of gateway into adrenal fatigue probably 3 to 4 years ago was training for a half marathon. And a half marathon's not that long, when you look at what a lot of people are doing with marathon training, with iron Man training, Half Iron Man training. I was training for this race and still doing other forms of exercise on top of that, so maybe running 20-25 miles a week, and then you know, my exercise for the day could have been anywhere from 60 to 90 minutes. A lot of that was steady state cardio or intervals- high intensity intervals, you know, to get my speed up. I'm not saying there aren't people out there who can probably handle that just fine. maybe the rest of the stressors in their life-and sometimes it's a cumulative or an additive effect, too right? Like you might have some people who lead very unstressful lives otherwise, their digestive health is great, all these other factors are great, so their, you know, impact of endurance training. And I know that we look down on endurance training a lot. I think maybe just you and I aren't very interested in it, so that's kind of the take that we have and, you know, I think we're allowed to have that.
And I think I have that because my real one bout with it was so detrimental to my health, that I'm like wow, you know, I wonder if other people are even realizing that it might be doing this to them. But, you know, they may have a different balance otherwise to that whole teeter totter effect, right? I mean, for me, maybe I had a lot of other things going on. I'm sure my digestion wasn't working great at the time. I still was not at that time eating a Paleo diet. Just start doing a gluten free thing. So I had a lot of other stressors going on, too, but I went and did a cardio kickboxing class after doing probably five mile training run. That five miles? That was not that much at the time. And I couldn't smile. Like I literally could not smile. and the only reason I did this class is because I thought they were fun. It was like dancing. And so that was a surefire sign that something was wrong, and I had no idea what it was, but it was exhaustion. And so people tend to ignore things, I think, but when your body is telling you something with, you know, that simple change in my mood and my energy. I just didn't know what it was. But I do think that there are definitely types of exercise that can do that.
I don't think we tend to see this type of thing from bodybuilders, you know, and I'm not saying that…maybe some of the, you know, hormone supplementation or whatever else might be going on might not be the best thing for people, but I think that typically, that steady state endurance activity does put more systemic stress on the body than something that's a lot more anabolic, like strength training. Or high intensity intervals, where you have a lot of more acute stresses, and then that stress is removed, and this is something I talk a lot about too where our body is wired up for an acute stress and then a period of long rest. So if you are a healthy person coming into a high intensity workout, then okay, this might be fine for you, to work out hard for 10 to 20` minutes, and then the next 24 hours basically you're resting and recovering. But somebody's who's already beat down and exhausted and feeling fatigue, 20 minutes of intense exercise may be too much for you. And every person is going to experience something different. And I think this where group classes that are like this is the one workout for everyone? I really strongly urge people to start to learn more about their own bodies' response, are they getting positive response after their workouts, are they feeling exhausted or are they making progress? You know, where do you fall in that?
And if you are not in a place where you think that those workouts are feeling good and right for you, if you feel beat up all the time, then that workout that's written on the board or whatever you had planned for yourself for that day might not be right for you that day. And, like, you know, there are times when I've walked into the gym and I've said, we're supposed to be doing this workout, and I'm not going to do the run. And I'm not trying to be a jerk, and I'm not trying to go against some programming that my coaches have put into place, and I just know, you know what? I'm going to just stand up for myself, and say, you know what? I can't do this today. I'm exhausted. I didn't sleep well last night, and I've been dealing with some adrenal issues. And you know what? A smart coach like mine says, okay, do you want to do something else? And I say, you know what, I'm just going to do the lift and that's it. And I'll do it along with everyone, and then I'm just going to do the lift part, and he said, okay. You know what? That's it. And so, you know, I think some people are just afraid to sort of stand up for what they feel might be right because a lot of times, you know, there are people who are just kind of wimping out on things that they don't want to do, and understanding where you fall within that range of just not wimping out but also trying to show off or think that you're stronger or better just because you did some hard work out when really you might not have been able to handle it that day.
So yeah. Long story short, I definitely think there's certain kinds of exercise that can contribute to this. I think that if you're dealing with the exhaustion, I really, really, really recommend Paul Chek's book, How to Eat, Move, and Be Healthy. I think-I've had several clients who have really needed to scale back on their workouts and some of them don't want to hear it from me, and some of them have not listened to what I've asked them to do and not scale back on it, or they scale back, and then they creep back into the workouts too soon, too intensely. And they experience backlash from that and continue to not make progress because we again, our expectations are like oh, well, if I back off for a month, that should be enough. I don't know how long is enough for every person. It's impossible to know until you start experimenting with some of it. But in How to Eat, Move, and Be Healthy, he talks about working in vs. working out, and really starting to do things that will build energy within your body and the way I kind of see it in this regard is that it will start to help balance out that neurotransmitter signal, so that you're not sending an imbalance to your adrenals, to say, you know, output the wrong amounts during the day. Really building up that energy in your body and keeping it for yourself, not constantly putting it out. That was a lot, but that's what I think about that. [laughs]
LIZ WOLFE: Yup. I like it. I think the same goes for, like stresswise, you have to remember that a marathon quote unquote, half marathon, CrossFit workout, even when it comes to food, Zone proportions or whatever, these are all for some people, like, they're arbitrary numbers. Like they're just that some kind of ideal for one reason or another, and you don't have to structure your life around these numbers. You don't have to run twenty-whatever miles. You don't have to do 21:15:9. If you know yourself well enough and, you know, embracing of that, you can say, I'm going to do what's right for me in this situation. so like you really do have to have the yin to the yang. And for these people, including myself and my husband, who are saying, yeah, we're doing relaxation, we're doing yoga. Let's make sure that that yoga is not Vinyasa yoga in a hundred fifty thousand degree room. Because I'm guilty of that, you know, like I've backed off on the CrossFit and realized that I was just adding in an hour and half 3 days a week of crazy intense yoga, so there really was no relaxation there….
DIANE SANFILIPPO:Yup.
LIZ WOLFE: And I think that started to cause me problems after awhile, so I love that…
DIANE SANFILIPPO:Yeah. Yeah, even planning out some workout schedules with my mom, it was like she told me stuff she could do every single day of the week. And I was like, well, where your rest day? And she was like, well…she said, well, those are just what are the options, I don't do them every single day. I was like, okay, good. You know, like at least a couple of days where you don't do any of this stuff. You know? Do some kind of meditation or just hanging out, you know? You don't have to go so hard all the time. People can actually do a little Google search for Zone exercises and get some YouTube videos and learn some of that, but I think that How to Eat, Move, and Be Healthy book-I'll link to it from the notes. I really like that book for assessing some of the issues that you're having with fatigue and then trying to figure out what at-home exercises you can do. They're literally like, don't require pretty much any equipment, maybe a Swiss ball, like a physio ball, maybe a foam roller. Some of it might be foam rolling, I don't remember exactly. I didn't grab the book off the shelf, but yeah.
What are some other questions around, sort of how did this stuff develop? Before I talk about some more what to do about it.
LIZ WOLFE: Well, yeah, I think you covered it really well, and we're rounding out on an hour right now, so I think you can probably just jump right into the nutrition treatment, kind of the protocol you're talking about.
DIANE SANFILIPPO:Okay. So I'm not going to spend too much time on the nutrition because pretty much everyone listening to this podcast is at a point where we probably know, we don't want to be eating sugar all day long. If you need to do a 21 Day Sugar Detox because you're eating, you know, clean Paleo, but you're still eating tons of fruit or you're chugging coconut water all day long and it's not a recovery for exercise, t's because you want something sweet. You know? Any blood sugar disregulation, all of that stuff. Food toxins, food allergens need to kind of get out. So I don't want to spend too much time on that. And we will kind of backtrack on a Paleo 101 because it seems like a lot of people want us to do a focus on that for one podcast.
But in terms of the lifestyle recommendations, sleep is absolutely number one. you know, the whole thing about your adrenals is the cortisol levels you're outputting throughout the day. If you're not sleeping well, your melatonin cycle, which as I said, the counter-regulatory hormone to cortisol. If your melatonin cycle doesn't have a chance to go its normal course, then you're setting up poorly for any possibility for a normal cortisol cycle. So if your sleep isn't good, working on sleep first is primo. I have-I think I have a post “Turn Down the Lights, Turn Up Your Metabolism” on my blog and I can link to that, and it has a whole bunch of sound sleep tips, things to do to get your sleep in line.
Other lifestyle factors-avoid draining people or draining situations and learn how to say no to things. You don't need to do everything people ask you to do. In fact, you know, saying yes to one thing a day is probably enough. And that could include work. People hate it when I tell them to get a new job, but I'm like, stop complaining. I don't know. There's only so much time you can handle a person complaining about something before it's like, so what are you going to do about it?
LIZ WOLFE: Exactly
DIANE SANFILIPPO:And even if you have a family to support, whatever it is, so either you change your situation or you change your thinking about it. So this is kind of the next step. If you're not enjoying your life, you can assess the following: whether you can 1. change the situation. 2. change yourself to fit the situation, which might mean changing your mindset or thoughts. Or number 3. leave the situation. You know, if a person is upsetting you, walk away. You know, if you can't stand your job, but you have to be in it for however much longer, you need to change your thinking. It's actually one of the things that our coach said two days ago after a workout. Yu know, when you're in the middle of something and this is not for those who are fatigued and failing, but you know, if you're strong and you're going through this workout, and you're just like, Oh, I suck. Change your thoughts. Literally change your thoughts. I don't know if this is a Brian Tracy quote or what, but I've heard this a million times before. “The conscious brain can only hold one thought at a time, so choose a positive thought.” Just like stop with the negative talk.
Don't overtrain. As I said, keep a gratitude list . that can be a really, really good way to recognize how many positive amazing things there are in your life instead of just focusing on the negative all the time. Play. Get out and play with your family, your friends, your pets. Do something fun. And I would read this post that I have: “Are You Driving Your Life Or Is Your Life Driving You? ” Again, that….
LIZ WOLFE: Nice.
DIANE SANFILIPPO:It's kind of about all these different factors, and you know, like, I've definitely had jobs that I've hated. Never for very long. I'll tell you that much. Because if I hate a job long enough, you sure as heck better believe I've started an action plan as to how I'm going to escape that job. And it's happened to me a couple of times in my life, and I've gotten out of them and started something different. And you know, I don't have a family that I need to support and I have family members of mine that are very supportive, and so maybe I'm lucky and I'm definitely grateful for all of that in its own right, but all of these things are things that I choose, and I don't try and focus on what's negative. I just make a plan to change it because I don't know what else to do. That's really all [laughs]. That's really the option, so I think that those are really important things for people to remember.
When I get through to some of the other nutrition issues, so keeping our standard sort of whole foods approach, but then looking at some things to do that are a little more specific. You may want to take a lower carbohydrate approach. I don't know that this is something that every person needs to do, but if your blood sugar regulation isn't good, sometimes taking that down a notch can really even things help. If you're not sure that that's a good approach for you, just keep it to some moderate level. Maybe you're getting 50 to 100 grams of carbohydrates a day, roughly speaking. If you're eating whole real foods, vegetables and some starchy tubers, you're going to come in at that range anyway. You don't need to measure all of it. Eating a wide variety of colors in your foods to make sure you're getting a lot of different nutrients in. Getting your omega-3/omega-6 balance in check, so really reducing that omega-6 fat intake. We want to make sure that we have enough anti-inflammatory fats in the system. You might find that when you are dealing with some adrenal issues, you might crave salts. That could be a sign or symptom, so adding some mineral salt to your food, even to your water, if you use any sort of filtered water, if you use distilled water for some reason. You could take Real Salt-Real Salt's one that I really like-and add a pinch of that to your water. Salting your food [xxx 1:00:06] whole salt. And you know, balancing your meals so the blood sugar regulation thing…you can judge the success of how well balanced the macronutrients were in your meals by how you feel entering into your next meal.
And this is really critical because if you're not working on blood sugar regulation, you cannot help and fix your adrenals. I will not do an adrenal test on a client until their blood sugar regulation is improved. If they come to me eating eight or nine times a day, and they're eating a piece of fruit 4 of those times, or they're just eating little sugary snacks, or they say they're starving, and they had to reach for something, that's not the time to test your adrenals. I don't need to test them. I know that you're messing up your entire endocrine function by pushing your insulin levels around. So getting your blood sugar regulation in line is absolutely key.
From there, know how I was saying fixing your adrenals or adjusting them is not the only way, but you do want to support the glands themselves. So foods that are high in vitamin C, like citrus, strawberries, kiwis when they're in season, cruciferous vegetables like Brussels sprouts, cauliflower, broccoli, kale, these are all cruciferous vegetables. Foods that are high in B vitamins like liver, generally well raised pastured meats and seafoods, some seeds can be useful, mushrooms are high in B vitamins. Foods that are high in magnesium: leafy greens, pumpkin and sesame seeds, or tahini, so you can grind them up if you want to. Salmon and halibut, also high in magnesium. Epsom salts baths are a way to get magnesium in as well, which I've been doing that regularly. And again foods high in omega-3 fats: salmon, walnuts, sardines, halibut, and I have what else here? Just keeping your range of micronutrients wide by getting in lots of different colors.
So some other helpful supplementation-I'm sipping down lots of water-just with stress, as I talked about getting these nutrients from your fooDiane Sanfilippo:vitamin C. You might want to be supplementing with vitamin C. What I'm not going to do is give everybody a dosage recommendation right now because I'm not doing anything prescriptive if I haven't worked with you and I haven't seen, you know, what your diet and lifestyle are, what your adrenal stress index shows. I can't tell you how much of things to take, but I can give some rough ideas of things that might be useful. But I do definitely recommend that people who think that they're really seriously dealing with this, get it tested. I have a bunch of practitioners that I can refer people to, and you can find a naturopath, sometimes a chiropractor in your area will do this. Any nutrition consultant is certified to do this kind of testing, too. But vitamin C, vitamin B5. The vitamin, a potent antioxidant, will help reduce- will help induce an anti-inflammatory response to, you know, prolonged exercise and stress. Vitamin B5, helping to activate the adrenal glands and you know, deficiency in B5 might result in some adrenal insufficiencies. So again, we want to just make sure that we're not, once we do start to try to balance out our adrenals, and balance out the messages we're sending to them, that our adrenals are well equipped. to handle that and come back to, you know, a normal level if they are outputting a higher or lower. So vitamin C, vitamin B5, a B Complex might be useful again just to support adrenal function and production. And as I said, magnesium is essential to the production of hundreds of enzymes and energy cycles throughout the body.
Some helpful herbs which is for the most part what I would be recommending are well-natural recommendations-er, supplements for people. Licorice root extract, if your cortisol is low, and this one that I really do think you need to test it to see where it's at, because sometimes you feel tired, but you might actually have a higher cortisol output at that time. But you can play around and tinker a little bit with licorice root extract or licorice root tea. I had one client who had a lot of success just supplementing with some licorice for a few months, and she kind of bounced back and dropped a pants size and was feeling a lot better just by doing that. So, you know, everyone's got a different situation, but licorice root extract is going to extend the half life of cortisol in your bloodstream, so you don't want to be taking that in sometime after, you know, 3 PM. But in the morning, you can do licorice root tea; it's actually pretty sweet. Or that extract, you can take that.
Phosphatidl serine or phosphorylated serine, which comes in a-called Seriphos, something that people can get online. That's something that can be helpful when your cortisol levels are too high. It can help to re-regulate that altered rhythm. It helps to regulate what's happening with your hippocampus. Again, this isn't stuff I would really tinker with unless you know what your levels are. Some other supports: l-theanine is a calming amino acid. It works by increasing GABA, which is an inhibitory neurotransmitter and it's a relaxer, creates a sense of well being in the brain. So people-some people may have heard of GABA as something you would take. You may or may not have. But that can be a useful one. Again, GABA on its own sometimes; it's a calming neurotransmitter, so I've had people who are like telling me they have anxiety and stressed out all the time, and GABA can be really useful. Melatonin is something you could do short term at bedtime. I don't know that it's something that I love. I know a lot of people lean on it or take it. I think in a very acute situation where you really need to sleep, if you are not going to have an addictive tendency towards it, or you don't feel like hung-over or sluggish after taking it, which is sort of how I felt when I tried to take it, then it might be okay for you in short term doses. But I wouldn't really lean on that too much.
Some other things that can be really helpful are adaptogenic herbs. And I think these are pretty easy for most people to take, pretty much anytime because what an adaptogenic herb does is it actually senses which direction you need balance. And so the herbs are where I would say, if you're just trying to support your system, getting some vitamins in and some herbs, you can't really go too far wrong with that, and you can't really mess yourself up with that. So some adaptogenic herbs are like ashwaganda root, ashwaganda leaf, ginseng, ginger root can really be helpful, or gingko biloba. These are all different adaptogens. Gaia Herbs has an adrenal support blend that's filled with adaptogens. Most adrenal support blends that you see out there are going to have herbs and adaptogens. They may have some B and C vitamins. They may have magnesium. I think a lot of people have tried like Natural Calm, possibly as a magnesium supplement. That's one form of magnesium. I think it's magnesium citrate. You may want to look at something like magnesium glycinate or magnesium maleate, which is a different form to help bring some calm to your brain. And as far as one other form of magnesium, I mentioned briefly before would be an Epsom Salts bath, which is also really good for muscle recovery, so I like that as well to just kind of help you calm down in the evening. Especially if you're drinking a drink at night is going to make you wake up to go to the bathroom, you don't want to be encouraging that too much.
What else? Those are-that's pretty much everything that I have on adrenal support. So what I'm doing for myself right now. My-I think I said my tests came back overall pretty low in some adrenal-some altered rhythm problems. I actually am taking…I'm taking a hormone precursor called pregnenolone. It's again I wouldn't say just go out and buy this. But because of the way my results came back and what I know to do for myself and also working with one of my colleagues to help me with my protocol, I'm taking some pregnenolone. You guys can kind of Google through stuff on it, read up on what it does, what it is. But it's a hormone precursor to kind of help reset a little bit of my brain chemistry. I had been working for a really long time on the food and lifestyle factors, and I just could not sleep through the night well. I'm still having trouble. I'll wake up early for no good reason. At like no matter what time I go to sleep, I'll wake up between 5 and 6 AM, and I really could sleep until 7. Like that would be fine, but without an alarm clock, I'm up before 6 pretty much every day. But I am taking some pregnenolone. I'm also taking some licorice root extract a couple times a day. And I'm taking an adrenal blend that's from a practitioner line called Designs for Health, that includes a bunch of the stuff I just talked about: some adaptogenic herbs, it includes B and C vitamins, little bit of-oh this is the new one I got. I got a new one to try that has a little bit also of adrenal glandular in it because I'm still feeling like I'm not quite there. It's been a month. I anticipate doing this for probably 3 to 6 months and I had been feeling before this, like, no joke from 12 to 6 PM like every day, like I could probably go to sleep at any given time. I'm sure people wouldn't guess it because I've been working my butt off for the last couple of years, but I've really been struggling and dragging. And the whole coffee on and off situation has been a real struggle because sometimes I feel like, you know what, I just can't make it through the work I have to do and I can't get through life this week without it. And then I hit a point where I realized that coffee actually made me feel worse for awhile. So that just happened a couple of days ago. I was like wow, I feel awful today. I need to not have this coffee, I need to make sure I'm falling asleep early. I'm like putting myself in bed by 9 o'clock, hoping to fall asleep by ten. It's really get serious, but when you realize how important it is to get to sleep, so that your whole rhythm can be set up properly for the next day. Like it's almost like you'll do anything [laughs] to be able to get yourself to sleep. So that's my protocol.
I think the last thing I'm taking evenings are-I've been taking some of that Seriphos that I mentioned which is a phosphorylated serine that's similar to Phosphatidl serine , but I guess it's just a slightly different form that your body does not have to put through one more process before it's usable, so similar, I think-this is an analogy I'm making. I don't know if this is exact or not. But similarly to the way some people take different forms of omega-3 fats, like the usable end form is DHA. Ideally and possibly some EPA. I think that's what the phosphorylated serine is, compared to the phosphatidl serine. I think it's more usable, more bioavailable. Anytime we can take some steps away from what's bioavailable to us when we're in sort of this depleted stressed state, I think it's probably better, and it's something both my practitioner friend, Mary Vance, my colleague. She and I work together on a bunch of things and I recommend a lot of people to talk to her. She specializes in female hormone disregulation, and also, Chris Kresser, I asked him what he liked for it. And he also, the Seriphos is what he recommended, so that's what I've been taking.
And you know, still working on the sleep, feeling much better throughout the day, not totally there yet, to the point where it's like wow, I feel great all day long. But I do notice that for me. If I am up and about and moving, like literally physically moving cortisol around my bloodstream by just moving around throughout the day, I definitely feel better than when I'm sitting, typing, working, writing. I feel very drained doing that. It's very funny to leave an office job and still be sitting most of the day. But at least I can get up and do other things when I want to. I'm definitely not complaining about it because I choose all of it, but I am still working on all of that. That's my current protocol.
LIZ WOLFE: All right.
DIANE SANFILIPPO:[laughs] I'm like, you're muted over there. I know you mute yourself just in case there's like barking dogs or husband coming in being like “Where are you? Hello?”
LIZ WOLFE: Ah, that did happen one time, didn't it? Wow.
DIANE SANFILIPPO:Wow. Yeah.
LIZ WOLFE: Yeah, pretty much. So during this time actually, I took a flute lesson and weeded my garden. I hope you don't mind.
DIANE SANFILIPPO:Awesome.
LIZ WOLFE: [laughs}
DIANE SANFILIPPO:You were also blending, I'm sure you were blending juices in your Vitamix and…I'm just kidding.
LIZ WOLFE: Yes, I was.
DIANE SANFILIPPO:I'm making that up entirely. Were there any questions that we didn't cover from Facebook that you think were kind of important ones or is that pretty-pretty much it? I know we're coming up on not much time so I wanted to make sure. Probably.
LIZ WOLFE: I think-I actually kind of like where we landed with this. And I'm assuming we'll have a bunch of more questions kind of inspired by this podcast. So…
DIANE SANFILIPPO:Mm-hmm.
LIZ WOLFE: we could probably wrap doing possibly like a second podcast based on follow-up questions and stuff like that because I think you hit on most people's concerns, but I'm sure they'll process them and kind of apply them to their own situations and be able to come up with some more questions that are related to it. So let's…
DIANE SANFILIPPO:Yeah, I think that's a good idea.
LIZ WOLFE: Yeah.
DIANE SANFILIPPO:Yeah, so when we put up the show notes from this, and I'll post about it kind of on that thread that we posted today. I want people to respond. Maybe we can just have them respond with questions in the comments there. But really ideally, getting submissions of questions through the podcast link on the site where it says “submit a question.” That's really the best place that we can keep sort of triage of our questions. but, you know, if you throw it into a comment, we'll try and wrangle it in. But I do want to make sure that we kind of try and answer questions on this, as best as I can. You know, I'm not, this is not the one subject that I'm the biggest expert on, but it is something I've researched a ton, and I'm dealing with. Something, you know, I think people can benefit a lot from just a basic understanding of how their body is working or not working. So cool. Let's dig into it more another time.
LIZ WOLFE: Sounds good, friend. I will talk to you….
DIANE SANFILIPPO:Mm-hmm.
LIZ WOLFE: Oh. we've got-we're recording. Maybe we should put that out here. We're recording with Jimmy Moore here in a couple of weeks. So people should look out for that podcast. Upcoming.
DIANE SANFILIPPO:Yeah, I don't know when. That'll be on his show…The Livin' La Vida Low Carb Show on iTunes. I don't know when it will air. he's got an amazing schedule that happens. And you know, one time I recorded with him and it aired a lot later, so I'm not sure. But we'll definitely tell people when we find out, we'll tell people when that's going up. So that should be fun. His podcast is awesome, too, if you haven't listened to it. He gets a lot of different, really amazing experts on it. And we're also going to be working on getting more guests on that have some recommendations for us to do that as well. People like the guests, so we'll work on getting a couple new people on, too.
LIZ WOLFE: Cool.
DIANE SANFILIPPO:Cool. All right until next time.
LIZ WOLFE: Bye-bye.
DIANE SANFILIPPO:Peace.
![]() Click here to submit questions.
Click here to submit questions.
Cheers!
Diane & Liz


Comments 16
Looks like the download mp3 is last weeks episode (14).
Oh! I see… I had trouble getting the download link for this episode and must have forgotten. I am still having trouble getting it but will fix as soon as I do! You can listen from this link as well, and possibly the “download this episode” link will work for you…?
http://www.blogtalkradio.com/balancedbites/2011/12/01/15-balanced-bites-podcast
Thanks Diane! Can’t wait to check out this weeks episode. Definitely interested in learning more on Adrenal Fatigue.
Thanks so much for this podcast! I was just diagnosed with early adrenal fatigue and was looking for more information. This gives me a lot to think about. Hopefully, after digesting all this great info, I’ll have some further questions to pose. 🙂
Why do you guys have to do that whole medical disclosure thing? If people actually stopped listening to their doctors and started listening to real people who know about nutrition (like you) the world would be a better place.
🙂
Diane,
What do you think of/know about functional diagnostics?
Cate
I would love to be able to download the graphics or find somewhere online to view them. I saw them really briefly on BlogTalk radio, but I couldn’t pause to get a good look or find a way to save them. I’ve been trying to wrap my head around adrenal fatigue for over a year, and I guess I need visuals when studying all these body systems!
I think many of them are available here: http://www.robbwolf.com/2012/04/09/real-deal-adrenal-fatigue/
Diane, your knowledge of health is such a treasure. Thank you.
Diane, your knowledge of health is such a treasure. Thank you.
I’ve had this podcast on my “suggested must listen to” list for some time now. After weeks of extreme stress syndrome, for lack of a better descriptor, I listened, there is so much insight here as to what has been happening to me and how to deal with it. I highly recommend this podcast as a must listen to series. Thank you for sharing your time and sourcing excellent speakers, like Diane, to help people find their way naturally without chemical interference.
I’ve had this podcast on my “suggested must listen to” list for some time now. After weeks of extreme stress syndrome, for lack of a better descriptor, I listened, there is so much insight here as to what has been happening to me and how to deal with it. I highly recommend this podcast as a must listen to series. Thank you for sharing your time and sourcing excellent speakers, like Diane, to help people find their way naturally without chemical interference.
Pingback: How The Brain Regulates Pain | D.I.G.
Hi Diane, I have been dealing with adrenal fatigue some time. I have recently considered taking a prohormone supplement and was interested that you have elected to take pregnenolone. I realise that you are unable to advise people over the internet but I was hoping you could explain why you chose pregnenolone, as well as the dose you chose to take. All the best and keep up the great podcasts
Josh
Pingback: My struggle with adrenal fatigue. ~ Real Food with Dana
Pingback: Adrenal Fatigue – The Aubrey Fam